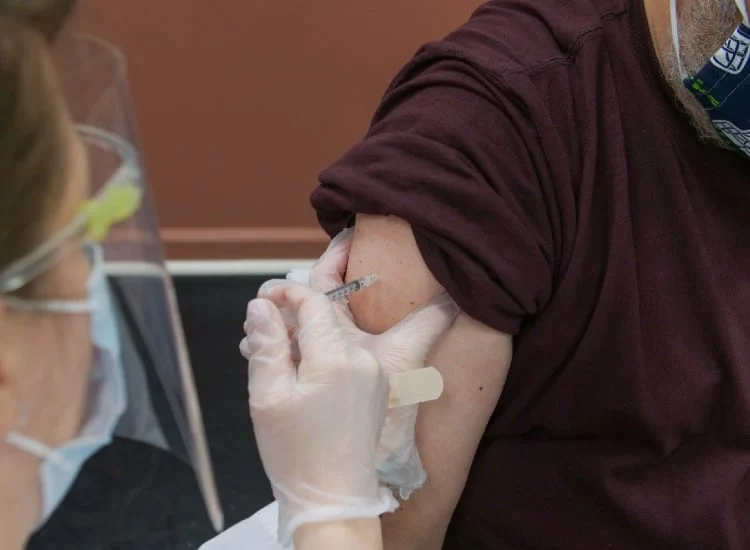
Living with Dementia: Supporting Your Loved One Following the COVID Vaccine

According to the Alzheimer’s Society 9 out of 10 deaths from coronavirus have been in people aged over 60. Due to the majority of people living with dementia being over the age of 65, it’s therefore understandable that the risk does increase for people living with a form of dementia. It isn’t just because of age though; confusion resulting from dementia can mean a person doesn’t understand the rules around social distancing, frequent handwashing and other COVID-19 measures, as well as the increased likelihood that someone living with dementia will have care inside their home from an outside source. These things can all increase the risk of coming into contact with the virus for someone who is living with dementia. With that in mind, we have put together things to consider when a loved one with dementia is considering the COVID-19 vaccination, including how to talk to them about the jab, during the event and what happens afterwards.
Talking to Your Loved One About the COVID Vaccine
When the lockdowns began, it would’ve been difficult for someone living with dementia to understand why their routine had suddenly changed. Despite them not necessarily remembering what they would regularly do from day to day depending on the severity of their condition, they may well have realised that things were suddenly different.
The same can now be the case for the vaccine. The fact that it is on television and in the papers on a daily basis doesn’t necessarily mean that your loved one will have fully understood the implications of the vaccine, and may therefore find it difficult to give their informed consent. You will know how well your loved one or customer is able to understand and follow conversations, so if you can, talk to them about the vaccine, but try to do so in non-alarming ways. Use short sentences and simple language to explain why it is important and what will happen if they have the vaccine.
Do your research
Where possible, you should do as much research as you can into the vaccines themselves so that you can be fully versed with the facts and can therefore answer the person’s questions. However, do ensure that the sources you’re using are credible, such as the NHS or Government websites.
Equally though, you should find out if the person has had vaccines before and if so, what the outcome was. For instance, have they been afraid when having previous vaccinations? Was this an expected level of fear or did it border on phobic? Did they have any side-effects after their previous vaccines? Were they expected side-effects or were they severe? This kind of research can arm the person with the facts and support them to make their decision, or instead support the decision-maker to make the most informed choice on their behalf. You can find out more about the benefits and risks of coronavirus vaccines here.
Make Sure They’re Comfortable
Choosing the right time to have the conversation about the vaccine can also make a huge difference to the outcomes of the conversation. Try to make sure you’re not talking to the person at a time when they traditionally prefer quiet; during their favourite television programme for instance, or when they would usually take a nap. To make sure that the person gets the most from the facts you’re trying to impart to them it’s important they’re as receptive as possible; so avoid times when they’re more likely to be hungry, tired or when time is short and you’ll have a much better chance of a positive reception. None of us feel at our best when hungry, thirsty or in a hurry so it makes sense that a person living with dementia won’t feel like having an in-depth conversation at those times either.
Listen to Their Concerns
If a person who’s living with dementia has concerns about receiving the vaccine, or are anxious because they haven’t yet received it, it’s important that you listen to their worries and make sure they know their feelings are validated. There is a lot of information about coronavirus in the media and we can be at risk of an overload of information if we try to take it all in, so if the person is confused and concerned about what they should do for the best, allow them to speak without interruption and say what is worrying them. Even if what they say is completely opposed to your own feelings about the vaccine it’s important you don’t try and change their mind; all you can do is listen and reassure them and try to discover the answers to their questions on reputable websites such as the NHS.
Helpful Questions and Phrases
You will be familiar with how your loved one or customer communicates when they have something they want to express, so it’s important to look out for those cues and to be patient. It’s sometimes tempting when caring for another to think we ‘know’ what they want to say, especially if they are having difficulty articulating the words, but it’s vital we don’t speak on their behalf or try to second-guess them. The British Red Cross have some useful advice on starting difficult conversations about the COVID-19 vaccines here including:
- Giving the person space to talk
- Actively listening to them and acknowledging their worries, questions and emotions
- Taking in what they are saying, and if you don’t understand asking them to clarify
You could also use visual prompt cards to assist the person if that is something you’ve done before but whatever method you use, ensure you’re being truthful.
For instance, saying ‘it won’t hurt’ may not be helpful, as some people commonly experience a sore arm after having the vaccine. Instead, say something like, “Your arm may feel sore, and you can get a headache or fever after the injection” but make sure they realise this isn’t definitely the case for everyone. As another example, if the person is unsure why they are having the vaccine, state that “it is so you are protected from the Coronavirus” and reassure them that they cannot get the virus from having the vaccine.
Also, it goes without saying that you should avoid alarming words such as ‘death’, ‘dying’ or ‘hospital’ for instance, or anything else that may cause the person’s anxiety levels to increase.
Give Them Time
It’s important that the person doesn’t feel rushed or pressured into making a decision about when, or indeed if, they want to have the vaccine. Ensure they have understood as best as you can and if in doubt, you could ask for assistance from the person’s medical practice or the NHS 111 service. If the person still has mental capacity, then they will have to give their consent to have the vaccine and this is why it’s so important that we ensure they’ve understood what they would be agreeing to. Ask the person directly if you can have their permission to arrange the vaccine for them in plain and simple language, for example “I would like your permission to give you the vaccine” or whatever is appropriate. Dementia UK recommends that, if the person is experiencing heightened anxiety or distress, rebook the vaccine at a different time and consider how you can support them next time.
Arranging Their Vaccination
If the person is registered with a GP then they should receive a letter, email, text or phone call inviting them to attend one of the clinics, surgeries or other locations where the vaccines are being given. If you or they feel they should’ve already received an appointment and they haven’t, check with their decision-maker or call their GP’s surgery, and ask when they should expect to receive it. It’s also important to remember that the vaccine is free. If you are asked to provide bank details, identification or to pay for the vaccine in any way then you should ignore the request. If you are concerned that the person living with dementia may have given this information already, then the NHS suggests you call Action Fraud on 0300 123 2040.
When the appointment arrives, make sure it is on a day when there is plenty of time to prepare the person and allow extra time to get to the location. Normally when a person attends the appointment, they are expected to go into the clinic alone to control the number of people there at any time. However, you should ask in advance whether you can accompany a person who is living with dementia to minimise their anxiety and confusion. According to the NHS, a carer will be allowed to go in to the appointment with their customer, but if in doubt, check first just to make sure.
Once inside, ask the person giving the vaccination if they can introduce themselves and if they are able to wear a clear visor rather than a mask so it reduces confusion for the person receiving the vaccine. It’s also vital to tell the staff if the person having the vaccine has ever had an allergic reaction to one before. Distracting the person while they are receiving the injection can also be a good tactic as they may not notice it so obviously then. You could distract them through conversation, singing, or just a reassuring touch to make them feel better, or take a favourite item with them to the appointment for added comfort.
After the Vaccine
Immediately after the vaccine, the person will be monitored for around 15 minutes to ensure they don’t exhibit a severe reaction. It’s important to keep the person calm and reassured during this period as while severe reactions are very rare, it’s essential that this monitoring takes place.
You should also be given a leaflet to take away with further information on it for any questions you or the person living with dementia may have once you get home. The person will be informed when they’re to be given a second dose of the vaccination several weeks later, so it’s important that all these steps are repeated when the second dose is to be administered.
Keep in touch
Coronavirus has made life especially challenging for people living with dementia, with closure of many local community activities and the socialising that they provided. If someone is living alone then this can make them at risk of further isolation unless they have a support bubble in place, so this is where having a carer come in and visit the person can be a lifeline. A Helping Hands carer can not only support with the practical everyday tasks that a person needs but they can also help someone to get online, make video calls and generally keep in touch with family and friends.
Monitor Their Behaviour and Emotions
Once they’re back home, it is essential to monitor the person for any unusual side-effects or strong reactions to the vaccine and you should familiarise yourself with what the difference is. If you have any doubts about what the person is telling you, or if you notice an unusual sign or symptom you should contact 111 immediately, or if they’re having difficulty breathing, call 999. The person may also be upset or angry that they’re having pain or don’t understand why they’re feeling tired, so being prepared in advance with answers to their concerns is sensible. Ultimately though, patience, consideration and planning will help the experience go as smoothly as possible.

Sarah joined Helping Hands in November 2016, working initially as a member of the Training and Development team due to her qualification in post-16 teaching. She has since moved into the Marketing team as a content writer, where she enjoys writing creatively for search and customer information.